Home » About Muco – Obstructive Pulmonary Diseases
The spectrum of lung muco-obstructive diseases that affect the airways, includes: COPD, Asthma, cystic fibrosis, primary ciliary dyskinesia (PCD), and non–cystic fibrosis bronchiectasis (NCFB), These diseases have the clinical features of cough, concentrated and thick sputum production, and episodic exacerbations that are often associated with a diagnosis of chronic bronchitis.
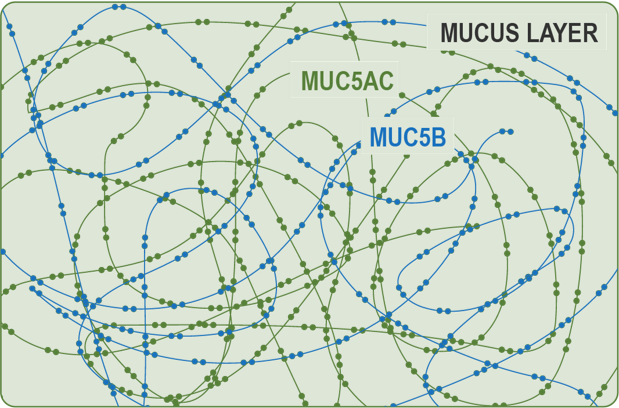
Human airway mucus is a hydrogel composed of approximately 98% water and 2% solids including high-molecular-weight mucin polymers. The two major synthesized and secreted respiratory mucins, MUC5B and MUC5AC, are physically very large proteins and a critical part of mucus.
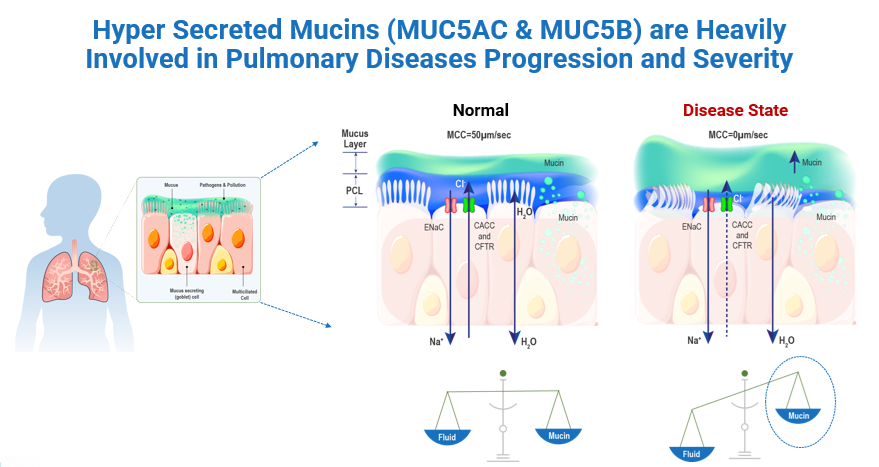
In healthy individuals, a well-hydrated mucus layer is transported rapidly (from the distal airways toward the trachea). In muco-obstructive diseases hyper-concentrated (dehydrated) mucus, failed mucus transport, and mucus adhesion to airway surfaces is observed. Mucus in the small airways cannot be cleared by cough and accumulates, forming airflow obstruction, infection, and inflammation.
MUC5AC concentrations are significantly and abnormally raised in muco-obstructive diseases like: COPD, asthma, subtypes of primary ciliary dyskinesia, and NCFB. MUC5AC elevated levels are consistent with the pathogenesis of the disease including airway obstruction, lung function deterioration, inflammation, exacerbations and mortality.

